COVID-19 is commonly associated with respiratory symptoms such as coughing and difficulty breathing.
However, gastrointestinal symptoms also begin to develop depending on how the body reacts to the virus.
Can covid cause stomach pain? Is there such as thing as gastrointestinal covid symptoms?
This article discusses common GI symptoms and when to know if it is associated with the disease.
COVID-19 Gastrointestinal Symptoms
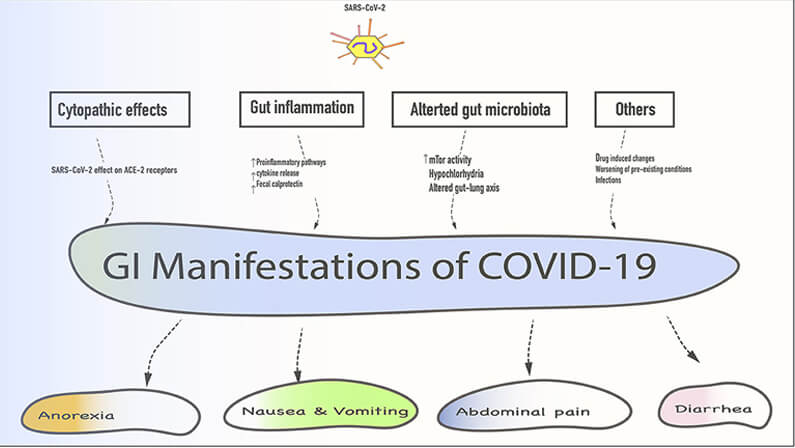
At the beginning of the pandemic, the most common warning signs of COVID-19 directly affect the respiratory systems. These include flu, coughing, and breathing problems that lead to pneumonia.
But as more and more studies emerge, researchers learn that the COVID-19 virus also penetrates multiple organs, resulting in various symptoms such as gastrointestinal distress.
In a study, experts found that COVID-19 patients may experience gastrointestinal problems while they deal with the viral disease.
The common GI complications are as follows:
- Diarrhea. Frequent bowel movements are associated with loose and watery bowels. It also comes with other symptoms like vomiting, abdominal discomfort, and nausea.
- Vomiting. Forceful movement in the abdominal wall causes the release of contents inside the abdomen. It also comes with saliva and an acidic taste.
- Belly pain. Stomach pain from constipation, irritable bowel syndrome, and discomfort from other organs.
Now you may ask, is stomach pain a symptom of COVID? Yes, it is possible especially if you have the above-mentioned warning signs.
Once you develop these symptoms, you can go immediately to Rapid Care ER to address your concern.
Our emergency doctors and nurses can accommodate you without having to wait for long. Call Rapid Care ER in our locations in La Porte and Katy, Texas, so we can attend to your emergency needs.
How COVID-19 causes GI symptoms
The COVID-19 virus destroys the body’s healthy cells and multiplies to attack the cells lining your airways. This process results in difficulty in breathing which leads to pneumonia.
In addition to these common symptoms, researchers have found that the illness can also harm the digestive system.
You may start experiencing the following common symptoms in the early days of the disease:
- Lack of appetite
- Loss of taste or smell
- Stomach upset which can last an average of 5 days
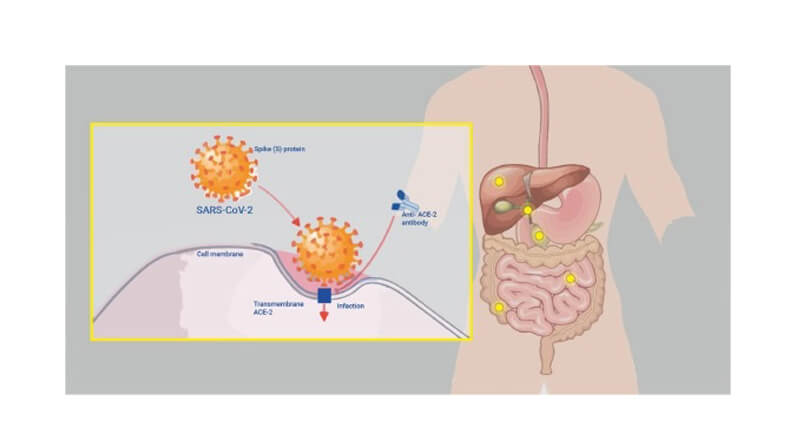
How Does COVID-19 Get into the GI Tract?
The virus enters the system through a protein that regulates blood pressure. It also regulates nutrient absorption in some organs, including the heart, kidney, and lungs. This protein is also found in the small intestine and the colon. When the virus reaches the gut lining, it turns leaky, which penetrates the system and causes GI problems.
If you are infected with the virus, traces of the COVID-19 virus should be able to appear in your stool test results.
Aside from usual diarrhea and vomiting, CT scans of patients with COVID-19 also present abnormalities in the bowel wall.
In some cases, clotting and thickening of the intestines and colon walls result in blood flow restrictions. Doctors may have to conduct surgery to treat these abnormalities and prevent more blood loss.
Gastrointestinal Complications In Critically Ill Covid-19 Patients
Aside from common GI symptoms that are easily treatable with over-the-counter medicines, other gastrointestinal distress can cause severe complications in other organs for critically-ill COVID-19 patients.
These may need further study from your doctors and more laboratory tests.
Acute liver injury and elevated transaminases
A condition where the liver stops functioning for days or weeks. This illness arises with no preexisting liver disease and may be triggered by a hepatitis virus or drug.
Acute liver injury may also cause elevated transaminases or high levels of enzymes found in the liver.
Acute cholecystitis
A condition widely present among critically-ill COVID-19 patients, acute cholecystitis is an inflammation of the gallbladder that develops when a gallstone blocks the cystic duct. Gallstones are made of cholesterol in the gallbladder.
Acute pancreatitis
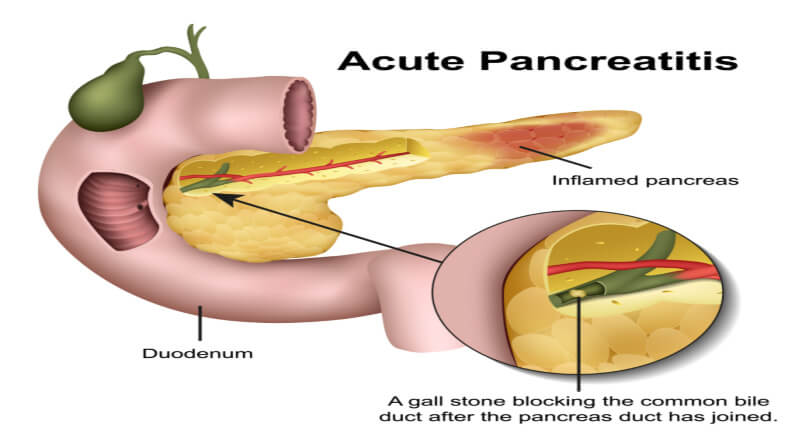
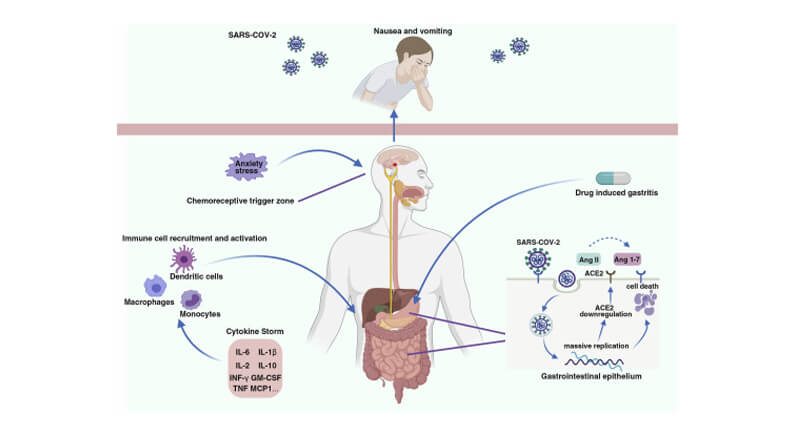
Experiencing COVID-19 stomach pain can be associated with this condition. This illness happens when the pancreas becomes swollen over a short period.
Ileus and feeding intolerance
Ileus is a temporary slowing of the digestive tract. It leads to a blockage in your intestine and prevents food, gas, and liquids from passing. GI complications may also result in feeding intolerance.
Acute colonic pseudo-obstruction
A disorder characterized by acute dilation of the colon and restricts the flow of intestinal contents.
Mesenteric ischemia
A condition that occurs when narrowed arteries prevent blood flow to your small intestine. If there is decreased blood flow, your small intestine can get damaged.
GI symptoms and disease outcomes
While GI symptoms can be mild and heal independently, it is still possible to develop other diseases, especially when associated with COVID-19.
- Acute respiratory distress syndrome. According to a study in 2020, there is a heightened risk of having acute respiratory distress syndrome if you have COVID-19. This disease is associated with low blood oxygen and usually comes with another complication.
- Noninvasive mechanical ventilation and tracheal intubation. COVID-19 patients may undergo ventilation and intubation to deliver oxygen during a critical stage.
- Acute infections. Children with COVID-19 and GI symptoms may experience severe cardiac impairments such as heart injury and heart failure.
- Kidney damage. About 30% of hospitalized COVID-19 patients may suffer from kidney injury, and some may be required to undergo dialysis.
- Barrett’s esophagus. A condition caused by acid reflux, this disease increases the risk of developing severe COVID-19 due to the esophagus as a potential gateway to infection.
Can COVID result in long-term Gastrointestinal Tract problems?
COVID-19 may leave long-term effects on various parts of the body, especially for people with other complications.
The case is also the same with the gastrointestinal tract. Recent studies reveal that the virus can linger in the GI tract for months.
The implications of this may include:
- Fatigue
- Nausea
- Depression
These symptoms may not be prominent and may not occur in all patients.
Meanwhile, you are more prone to complications if you have an existing GI problem such as Inflammatory Bowel Disease (IBD).
Taking immunosuppressant steroids, a type of medication for IBD poses a higher risk for complications from COVID-19 should you get infected with the disease in the future.
What To Do When you experience COVID-19 and GI symptoms
If you experience vomiting, nausea, and diarrhea, you need to take precautionary measures, especially if you are not confirmed with COVID-19 yet.
Here’s what you can do at home when you have stomach pain COVID symptoms:
- Stay home. Resist the urge to go out if you already have disease symptoms. Isolate as soon as possible to prevent others from getting infected.
- Isolate. Have a separate bedroom and bathroom if you experience COVID-19 symptoms to reduce the risk of transmission should you have the virus.
- Observe hand hygiene. Always wash your hands with soap and water whenever you go to the bathroom or eat food.
- Get enough rest. Take time to sleep and rest well. Avoid doing heavy activities that may trigger pain in your abdominal area.
- Take over-the-counter medication. Medicines such as loperamide can be a simple covid gastrointestinal treatment for diarrhea. Meanwhile, antihistamines like diphenhydramine are proven to reduce nausea. Take these medicines once you experience the symptoms.
- Hydrate. Frequent diarrhea and vomiting result in loss of fluids in the body. Drink lots of fluid like water and juices to keep yourself from dehydration. You can drink liquid with broth or salted crackers.
- Eat a bland diet. Replenish your body with carbohydrates by eating bananas, oatmeal, baked potatoes, white rice, or applesauce. This food also limits your urge to poop.
While having GI symptoms does not necessarily mean you have COVID-19, you need to get tested if you know you were in contact with someone who tested positive.
To know if you have COVID-19, drive to Rapid Care ER for immediate testing. Rapid ER provides fast and accurate tests to confirm if you have the disease or not. You can get the result in just minutes; from there, our emergency doctors will have to decide what type of treatment you need.
Treatment for COVID and Gastrointestinal problems
Most COVID-19 cases that come with common GI symptoms are mild. Diarrhea and vomiting may go away after a few days if treated with over-the-counter drugs, rest, hydration, and a proper diet.
However, there are instances when the virus can cause inflammation in the colon called colitis. Symptoms of this include bleeding stools and diarrhea.
If the bleeding lasts more than two days, go to an emergency room for immediate laboratory testing.
The doctor may also advise an immediate colonoscopy to determine the cause of the bleeding and the amount of blood loss.
When to go to an emergency
If you begin to develop extreme abdominal pain associated with COVID-19 symptoms such as difficulty breathing, go to the nearest emergency room for urgent treatment.
RapidCare ER can provide immediate medical care if you experience combined COVID-19 and gastrointestinal symptoms.
Our emergency doctors and staff are ready to assist you with any medical need, especially if you have COVID-19 symptoms that require urgent care.
We provide COVID-19 testing, both RT-PCR and antigen tests, to detect whether you have the virus or not. If you have the virus, we can immediately secure an isolated room for you and provide a dedicated team to look into your condition.
If you turn out negative, we will still proceed with other examinations in our laboratory to find out what causes your gastrointestinal distress. Our lab results come out in less than an hour, giving your doctor immediate information about your condition.
Call Rapid Care ER today or visit our locations in La Porte and Katy, Texas, for all your emergency needs.